In an era where desk jobs and digital devices dominate our lives, wrist pain exercises have surged in popularity as a go-to solution for alleviating discomfort that affects millions worldwide. If you’re experiencing nagging wrist pain that hinders typing, lifting, or even basic hand movements, incorporating targeted exercises can be transformative. Backed by physiotherapy principles, these routines not only provide immediate relief but also build long-term resilience.
Decoding Wrist Pain: What It Means and Why It Happens
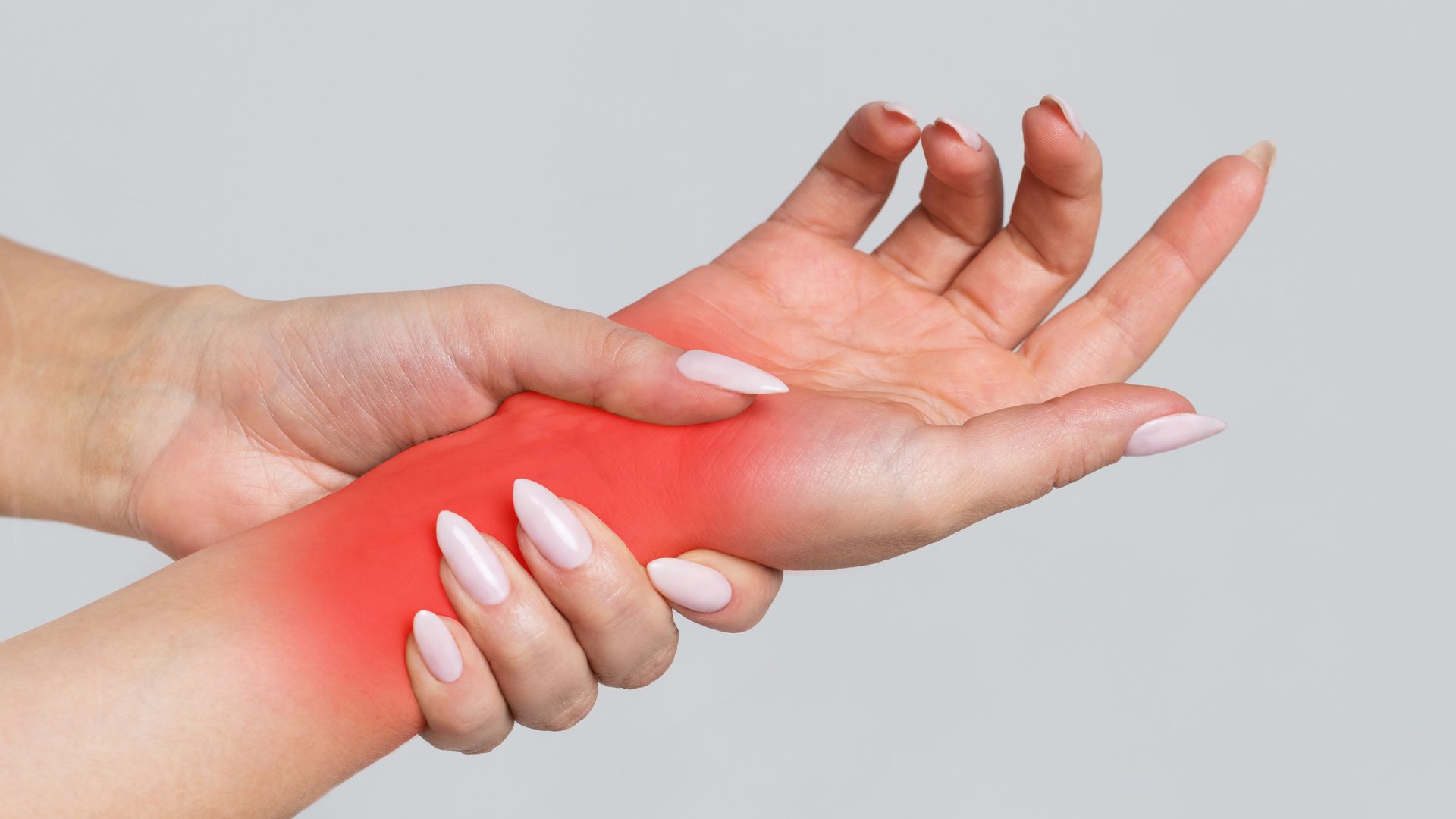
Wrist pain is more than just a fleeting ache; it’s often a signal of imbalance in the intricate network of bones, tendons, ligaments, and nerves that form the wrist joint. Defined as discomfort or soreness in the area connecting the forearm to the hand, it can range from mild irritation to debilitating sharpness, impacting grip and dexterity. Chronic wrist pain, persisting beyond a few weeks, typically arises when repetitive motions or poor ergonomics strain these structures, leading to inflammation or wear.
The wrist comprises eight small carpal bones arranged in two rows, supported by tendons for movement and ligaments for stability. When overloaded, this setup can falter, manifesting as pain that worsens with activity. Recognizing this early empowers proactive management through wrist pain exercises, which restore balance without invasive interventions.
Identifying Common Triggers of Wrist Discomfort
Pinpointing causes is crucial for effective relief. Repetitive strain injury (RSI) is a primary offender, often from prolonged keyboard use or assembly line work, inflaming tendons and causing conditions like tendinitis. Carpal tunnel syndrome (CTS) occurs when the median nerve is compressed in its narrow passageway, triggered by swelling from repetitive flexion. Arthritis, including osteoarthritis from age-related cartilage breakdown or rheumatoid arthritis from immune responses, erodes joint surfaces, leading to stiffness and swelling. Post-injury effects, such as from falls or sports, can also linger if healing is incomplete.
These triggers highlight why wrist pain exercises are essential, they address root issues like muscle weakness or tightness, preventing escalation into chronic problems.
Spotting Symptoms and Seeking Timely Diagnosis
Symptoms vary but commonly include throbbing pain during wrist movement, tenderness to touch, and reduced range of motion. You might notice swelling, a clicking sensation, or numbness extending to fingers, especially in CTS cases. Weakened grip strength can make holding objects challenging, affecting productivity and leisure.
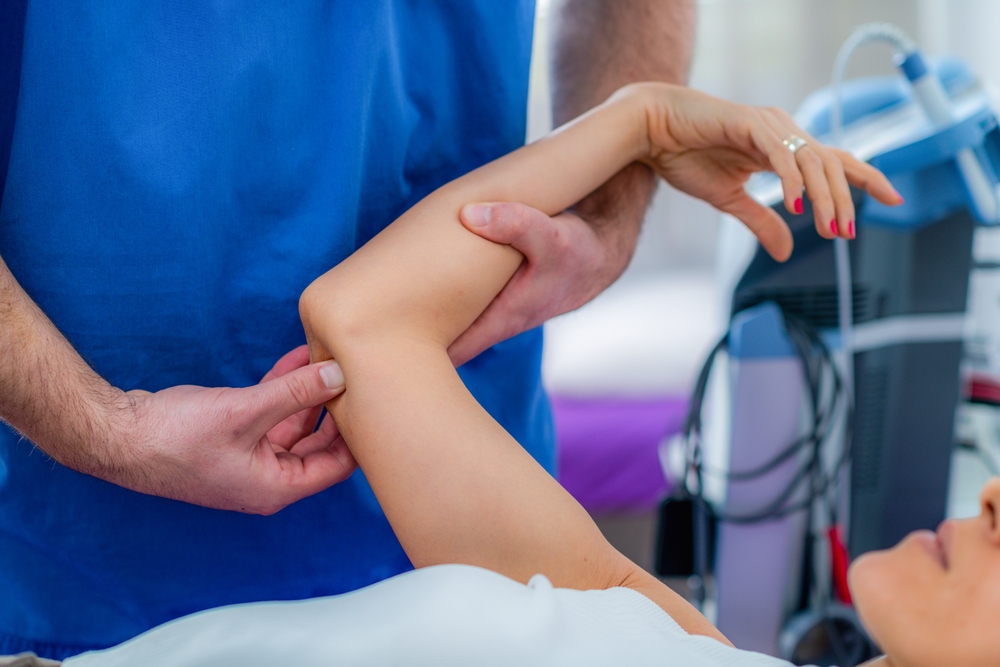
Diagnosis involves a clinical evaluation: assessing pain patterns, testing nerve function with maneuvers like tapping the wrist, and possibly imaging to rule out fractures. Early detection through these steps ensures wrist pain exercises are tailored, maximizing efficacy and minimizing downtime.
The Power of Early Action in Wrist Pain Management
Acting swiftly can halt progression. Untreated pain may lead to compensatory overuse of other joints, like the elbow, or permanent nerve damage. Starting wrist pain exercises promptly, ideally under professional guidance, can reduce symptoms by up to 50% in initial weeks, fostering better posture and habits for sustained health.
Core Wrist Pain Exercises
Physiotherapy-inspired wrist pain exercises form a topic cluster of stretches, strengthens, and mobilizations. Perform them gently, 2-3 times daily, holding each for 20-30 seconds without forcing pain.
Flexibility-Focused Stretches
Begin with wrist flexor stretch: Extend your arm forward, palm up, and use the opposite hand to gently pull fingers back toward your body, feeling a pull along the inner forearm. This targets tight flexors common in desk workers. Conversely, the extensor stretch involves palm down, pulling fingers downward to elongate the top forearm muscles, easing RSI tension.
Strengthening Routines
Incorporate prayer stretch: Press palms together at chest level, elbows out, then lower hands toward waist while keeping palms connected, stretching wrist undersides. For power, try fist clenches: Start with hand open, slowly form a fist, hold, then release, repeat 10 times to boost grip without strain. Wrist curls using light weights (or a water bottle) involve palm-up forearm on a table, curling wrist upward, then lowering slowly for controlled strengthening.
Mobility Enhancers
Nerve glides for CTS: Extend arm, fingers straight, then bend wrist back while tucking thumb in, sliding the nerve to reduce compression. Circle wrists clockwise and counterclockwise to improve joint lubrication and range.
This cluster ensures balanced recovery, combining elements for comprehensive relief.
Advantages of Consistent Exercise Practice
Regular wrist pain exercises yield benefits like enhanced blood flow, reduced inflammation, and stronger supporting muscles, often leading to 70% symptom improvement per studies. They promote independence, cutting reliance on meds, and enhance overall upper body coordination.
Proactive Prevention for Lasting Wrist Wellness
Prevent pain by ergonomically adjusting workspaces, keep wrists neutral, use supportive tools, and integrate breaks with quick stretches. Maintain a nutrient-rich diet for joint health, and warm up before activities.
Wrapping Up: Your Path to Pain-Free Wrists
Embracing wrist pain exercises offers a straightforward, empowering route to relief, blending simplicity with proven results for everyday resilience. Commit to these routines, and watch discomfort fade.For expert guidance, Physio Asia Therapy Centre, established since 2006, provides cost-effective, evidence-based physiotherapy services with integration of state-of-the-art technology and skillful implementation. Their specialized programs can personalize your journey to optimal wrist health.