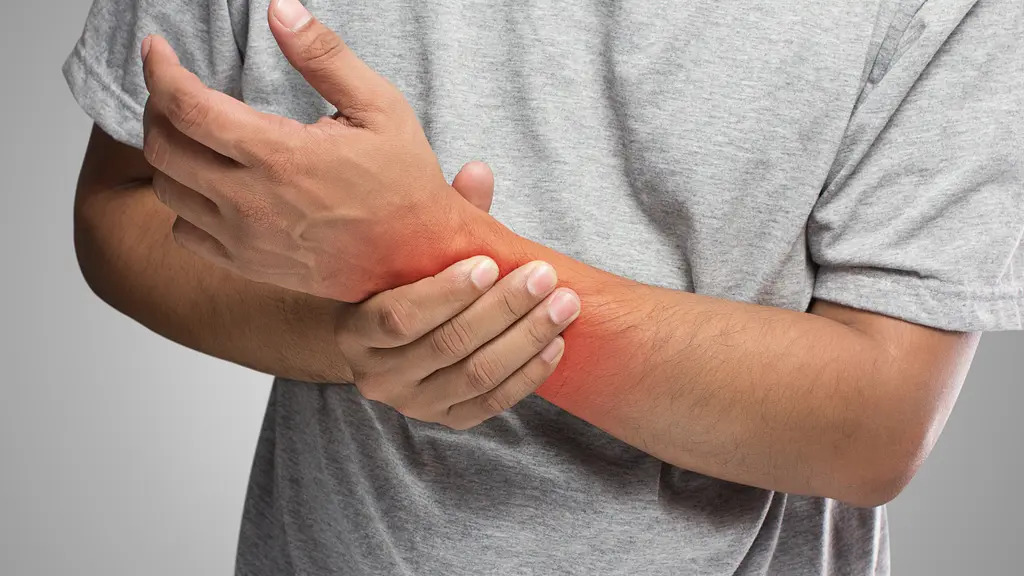
Wrist pain is a common and often debilitating condition that can significantly impact daily activities and quality of life. From typing at a computer to engaging in sports or even performing simple household tasks, a healthy wrist is essential for function and independence. While many people may initially dismiss wrist pain as a minor inconvenience, failing to address it can lead to chronic discomfort, loss of strength, and long-term dysfunction. Physiotherapy offers a highly effective and evidence-based approach to not only managing but also preventing and relieving wrist pain, providing a path to lasting recovery and improved mobility.
Understanding the Common Causes of Wrist Pain
The wrist is a complex structure composed of eight small carpal bones, two forearm bones (the radius and ulna), and an intricate network of ligaments, tendons, and nerves. Due to its complexity and frequent use, the wrist is susceptible to a wide range of injuries and conditions. A thorough understanding of the potential causes is the first step toward effective treatment.
- Repetitive Strain Injuries (RSI): This is one of the most frequent causes of wrist pain, resulting from continuous and repetitive movements. Activities such as typing, using a computer mouse, assembly line work, or playing certain sports (e.g., tennis, golf) can lead to inflammation and damage to the tendons and muscles.
- Carpal Tunnel Syndrome: A well-known condition that arises from the compression of the median nerve as it passes through the carpal tunnel in the wrist. This compression can cause pain, numbness, tingling, and weakness in the hand, thumb, and fingers, often worsening at night.
- De Quervain’s Tenosynovitis: This is an inflammation of the tendons on the thumb side of the wrist. It’s often caused by repetitive motions involving gripping or pinching, making it common in new parents (from lifting a baby), gardeners, and individuals who engage in frequent, forceful thumb movements.
- Sudden Injuries: Acute injuries, such as falling on an outstretched hand (FOOSH), can lead to wrist sprains, strains, or even fractures of the scaphoid bone or distal radius. These injuries require immediate medical attention and structured rehabilitation.
- Arthritis: Both osteoarthritis and rheumatoid arthritis can affect the wrist joints. Osteoarthritis is typically a “wear and tear” condition, while rheumatoid arthritis is an autoimmune disorder that causes chronic inflammation of the joints.
The Physiotherapy Approach: A Personalized Path to Relief
Physiotherapy is a holistic and non-invasive treatment option that targets the root cause of wrist pain. Unlike relying solely on medication or temporary fixes, physiotherapy focuses on restoring function, reducing pain, and preventing future injuries. The process begins with a detailed and comprehensive assessment.
Initial Assessment and Diagnosis
A skilled physiotherapist will start by taking a thorough subjective history, asking questions about the onset of the pain, its location, the types of activities that aggravate it, and any previous injuries. This is followed by a physical examination, which includes:
- Observation: The therapist will visually inspect the wrist and hand for any swelling, redness, or deformities.
- Movement Testing: Active and passive range of motion tests are performed to assess the wrist’s flexibility and identify any restrictions.
- Strength Testing: Grip strength and other specific muscle tests are conducted to evaluate muscle weakness.
- Special Tests: The physiotherapist will perform specific tests to diagnose conditions like Carpal Tunnel Syndrome (e.g., Tinel’s test or Phalen’s test) or De Quervain’s Tenosynovitis (e.g., Finkelstein’s test).
- Neurological Assessment: This evaluates nerve function to check for any nerve entrapment or compression.
This detailed assessment allows the therapist to accurately diagnose the condition and develop a customized treatment plan tailored to the individual’s needs and goals.
Core Treatment Modalities in Wrist Pain Physiotherapy
The treatment plan for wrist pain typically involves a combination of hands-on techniques, therapeutic exercises, and specialized modalities.
1. Manual Therapy
Manual therapy involves a variety of hands-on techniques performed by the physiotherapist to reduce pain and improve joint function. These may include:
- Joint Mobilization: Gentle, controlled movements applied to the wrist joints to reduce stiffness and improve range of motion.
- Soft Tissue Mobilization: Techniques such as massage and myofascial release to relieve tension in the muscles and tendons of the forearm and hand, improving blood flow and reducing pain.
- Nerve Gliding Exercises: These are gentle movements designed to help nerves, such as the median nerve in carpal tunnel syndrome, move more smoothly and reduce irritation.
2. Therapeutic Exercises
A cornerstone of physiotherapy is the prescription of a structured exercise program. These exercises are crucial for long-term recovery and prevention.
- Range of Motion Exercises: Gentle stretches and movements to improve flexibility and combat stiffness. Examples include wrist circles, wrist flexion, and extension stretches.
- Strengthening Exercises: As pain subsides, the focus shifts to strengthening the muscles of the wrist and forearm. This can involve using a light weight, a resistance band, or a stress ball to improve stability and endurance.
- Proprioception Exercises: These exercises improve the wrist’s sense of position and movement, enhancing coordination and balance to prevent re-injury.
- Stretching: Specific stretches for the wrist flexors and extensors help to maintain flexibility and reduce muscle tightness, which can often contribute to pain.
3. Physical Modalities
Physiotherapists also utilize various physical modalities to complement manual therapy and exercises. The Physio Asia Therapy Centre, for example, is known for its use of advanced, evidence-based technologies.
- Radial Shock Wave Therapy: This therapy uses high-energy sound waves to stimulate blood vessel formation and tissue repair, making it effective for chronic tendon issues.
- Laser Therapy and Ultrasound Therapy: Both use energy to penetrate deep into tissues, promoting blood supply, reducing inflammation, and accelerating the healing process.
- Cryotherapy: The application of cold therapy helps to numb pain and reduce inflammation, particularly in the acute stages of an injury.
- Wrist Guards and Dynamic Taping: These are used to provide support to the joint, relieve muscle tension, and help manage swelling during the recovery period.
The Benefits of Physiotherapy for Wrist Pain
The comprehensive approach of physiotherapy provides numerous benefits that go beyond simple pain relief.
- Long-Term Relief: By addressing the underlying cause of the pain, physiotherapy offers a more sustainable solution than temporary fixes like medication.
- Improved Mobility and Strength: Restores the full range of motion and strengthens the supporting muscles, allowing individuals to perform daily tasks without difficulty.
- Prevention of Recurrence: Through education on proper body mechanics, ergonomics, and an ongoing exercise program, physiotherapy empowers individuals to prevent future episodes of wrist pain.
- Non-Invasive and Safe: It provides an effective alternative to surgery and other invasive procedures, with a focus on natural healing and rehabilitation.
For anyone experiencing wrist pain, seeking professional help is a crucial step. Early intervention and a well-structured physiotherapy program can make a significant difference in the recovery timeline and overall outcome.
In conclusion, managing and relieving wrist pain through physiotherapy is an effective and comprehensive strategy for anyone suffering from this common ailment. By combining expert assessment, manual therapy, therapeutic exercises, and advanced physical modalities, physiotherapy addresses the root cause of the problem and provides a personalized pathway to long-lasting relief and improved wrist function. The journey to recovery is not just about treating the symptoms but about rebuilding strength, restoring mobility, and empowering individuals with the knowledge to maintain wrist health in the long run. Physio Asia Therapy Centre is an award-winning clinic dedicated to providing efficient, effective, and evidence-based physiotherapy and rehabilitation services in Singapore.