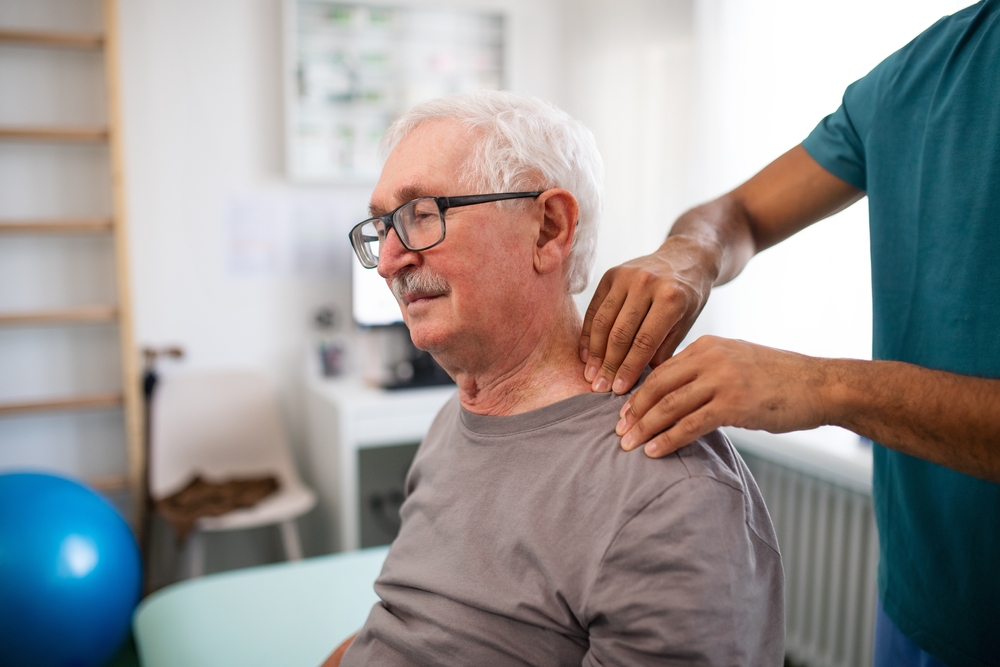
Neck pain is a pervasive issue in the modern world, affecting millions of people and significantly impacting their quality of life. From the chronic ache of the neck due to excessive screen time to the sudden, sharp pain from an injury, the discomfort can be debilitating. While many seek temporary relief through painkillers or massages, a more sustainable and effective approach lies in physiotherapy for neck pain. This article will delve into the critical role of professional physiotherapy, outlining specific exercises and treatment methodologies that not only alleviate pain but also address the root cause, leading to long-term relief and improved function.
Understanding the Anatomy of Neck Pain
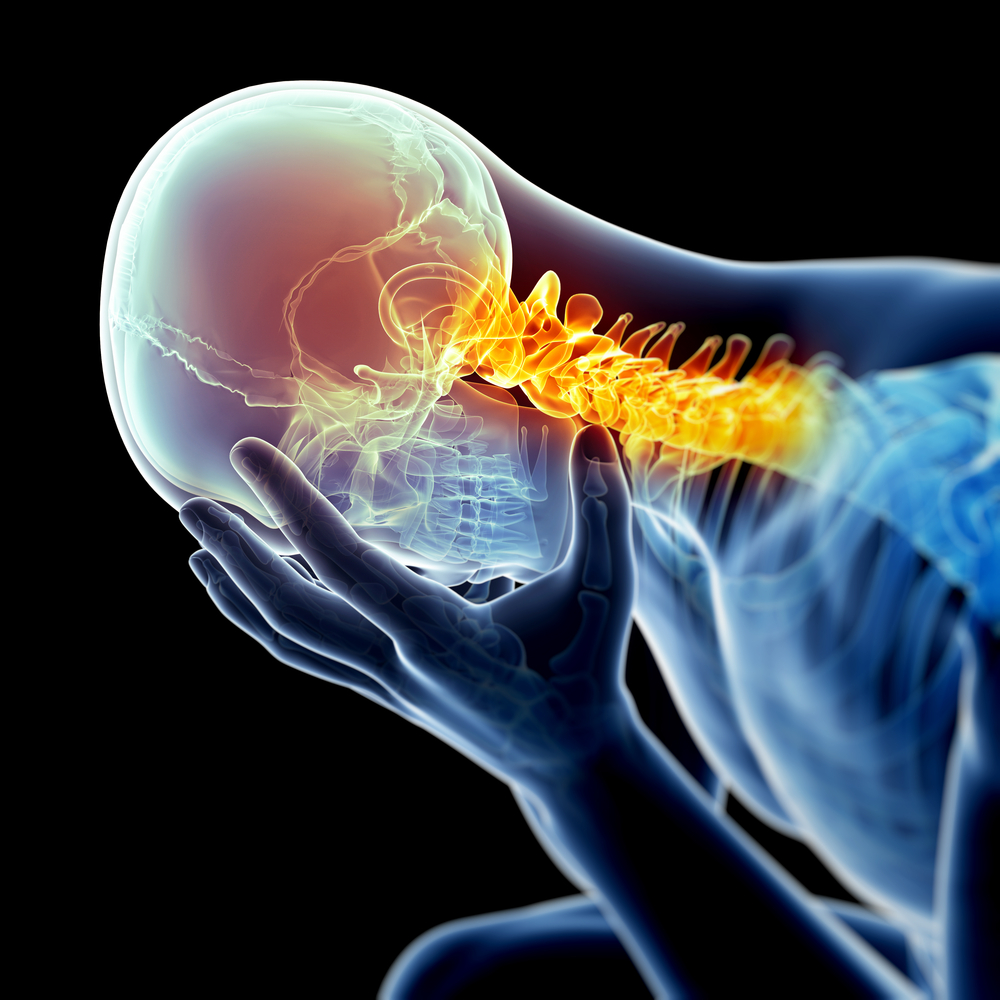
To truly understand how physiotherapy works, it’s essential to first grasp the anatomy of the cervical spine. The neck is a complex structure of bones, muscles, nerves, ligaments, and tendons. Its primary function is to support the head, which can weigh up to 12 pounds, while allowing for a wide range of motion. When this delicate balance is disrupted—whether by poor posture, muscle strain, or injury—the result is pain and stiffness. Physiotherapy for neck pain is designed to restore this balance, targeting the underlying issues rather than just masking the symptoms. It’s an evidence-based approach that combines passive and active treatments to promote healing and strengthen the supporting structures of the neck.
The goals of a comprehensive physiotherapy program are multifaceted. First, the immediate objective is to reduce pain and stiffness, creating an environment where healing can begin. This is often achieved through a combination of manual therapy and passive modalities. Second, the focus shifts to improving the head and neck’s range of motion. Restricted movement is a common symptom of neck pain, and a physiotherapist uses targeted stretches and mobilisations to restore flexibility. Finally, and most importantly, the program aims to strengthen the muscles that support the neck. By developing dynamic strength and stability, the neck becomes more resilient to future strain, and strategies are developed to prevent pain from recurring.
The Foundation of Relief: Targeted Physiotherapy Exercises
The core of a successful physiotherapy plan is a series of specific exercises tailored to the individual’s needs. These exercises are not random movements; they are designed to target and strengthen the deep cervical muscles that are often dormant or weakened in individuals with chronic neck pain.
One of the most effective and professional programs for addressing this issue is the SCORES – Spinal Core Stability Program. This program is designed to activate and strengthen the deep stabilising muscles of the spine, not just the superficial ones. The logic is simple yet profound: the stability of your neck is directly linked to the strength of your core. If the deep core muscles are weak, the body compensates by overworking the superficial muscles in the neck and shoulders, leading to strain, fatigue, and pain.
The SCORES program focuses on a three-pronged approach:
- Muscle Activation: The program uses specialised techniques to “wake up” the deep upper cervical/neck muscles. These are the muscles that provide intrinsic stability to the neck joints. By learning to activate them consciously, you can take the strain off the overworked surface muscles.
- Core Stability: SCORES extends beyond the neck, addressing the entire spinal core. It teaches patients how to control their diaphragmatic breathing and engage their deep abdominal and back muscles. This integrated approach ensures that the entire spine is supported, reducing the overall load on the neck. The use of specialised equipment, such as the Achievo Core Stability trainer, plays a crucial role in this phase. This device provides real-time biofeedback, allowing patients to see and feel the effective activation of these deep muscles, which is a key component of effective treatment.
- Functional Integration: The final stage involves integrating these new movement patterns into daily activities. A physiotherapist helps patients learn to maintain proper posture and use their newly strengthened core muscles during everyday tasks like sitting at a desk, lifting objects, and even sleeping. This phase is what makes the relief from physiotherapy long-lasting, as it turns good habits into second nature.
Beyond the SCORES program, a comprehensive physiotherapy plan will also incorporate a variety of other exercises, each serving a specific purpose in the journey to recovery.
- Stretching and Mobility Exercises: Gentle stretches for the neck, shoulders, and upper back are crucial for restoring a full range of motion. Movements like neck rotations, side bends, and chin tucks help to lengthen tight muscles and reduce stiffness. A physiotherapist will guide you on the proper form to prevent further injury and ensure the stretches are effective.
- Strengthening Exercises: As pain subsides, the focus shifts to strengthening. This can include isometric exercises, where you hold a position without movement, and resistance training using bands or light weights. These exercises build endurance and strength in the neck muscles, making them more resilient to the stresses of daily life.
- Postural Training: Often, the root cause of neck pain is poor posture. A physiotherapist will assess your posture and provide tailored guidance on how to sit, stand, and move in a way that minimises strain on your neck. This might involve adjustments to your workstation, advice on sleeping positions, or simple cues to remind you to hold your head in a neutral position.
- Manual Therapy: Physiotherapists also use a hands-on approach called manual therapy. This includes joint mobilisations to improve the movement of stiff neck joints and soft tissue massage to release tension in tight muscles. These techniques can provide significant immediate relief, allowing you to perform the active exercises more effectively.
Why Expertise Matters in Physiotherapy Care
A professional physiotherapy clinic embodies all these principles. The information and treatment you receive are based on the expertise of licensed professionals who have dedicated years to studying the musculoskeletal system. Their experience comes from treating countless patients with varying degrees of neck pain, allowing them to develop a deep understanding of what works. Their authority is established by their professional certifications and the results they achieve with their clients. Ultimately, this builds trust, as you can be confident that you are receiving a safe, effective, and evidence-based treatment plan. So, choosing a reputable physiotherapy center is a critical step in your recovery journey. So, choosing a reputable physiotherapy center is a critical step in your recovery journey.
Conclusion
In conclusion, relying on a professional physiotherapy center for neck pain is the most effective long-term solution. By addressing the underlying muscular imbalances and functional deficits, physiotherapy goes beyond temporary relief to provide lasting recovery. The combination of targeted exercises, manual therapy, and patient education empowers individuals to take control of their health and prevent the recurrence of pain. Through programs like SCORES and a personalised approach, physiotherapists offer a path to a life free from chronic neck discomfort. The Physio Asia Therapy Centre is providing efficient, effective physiotherapy services in Singapore.